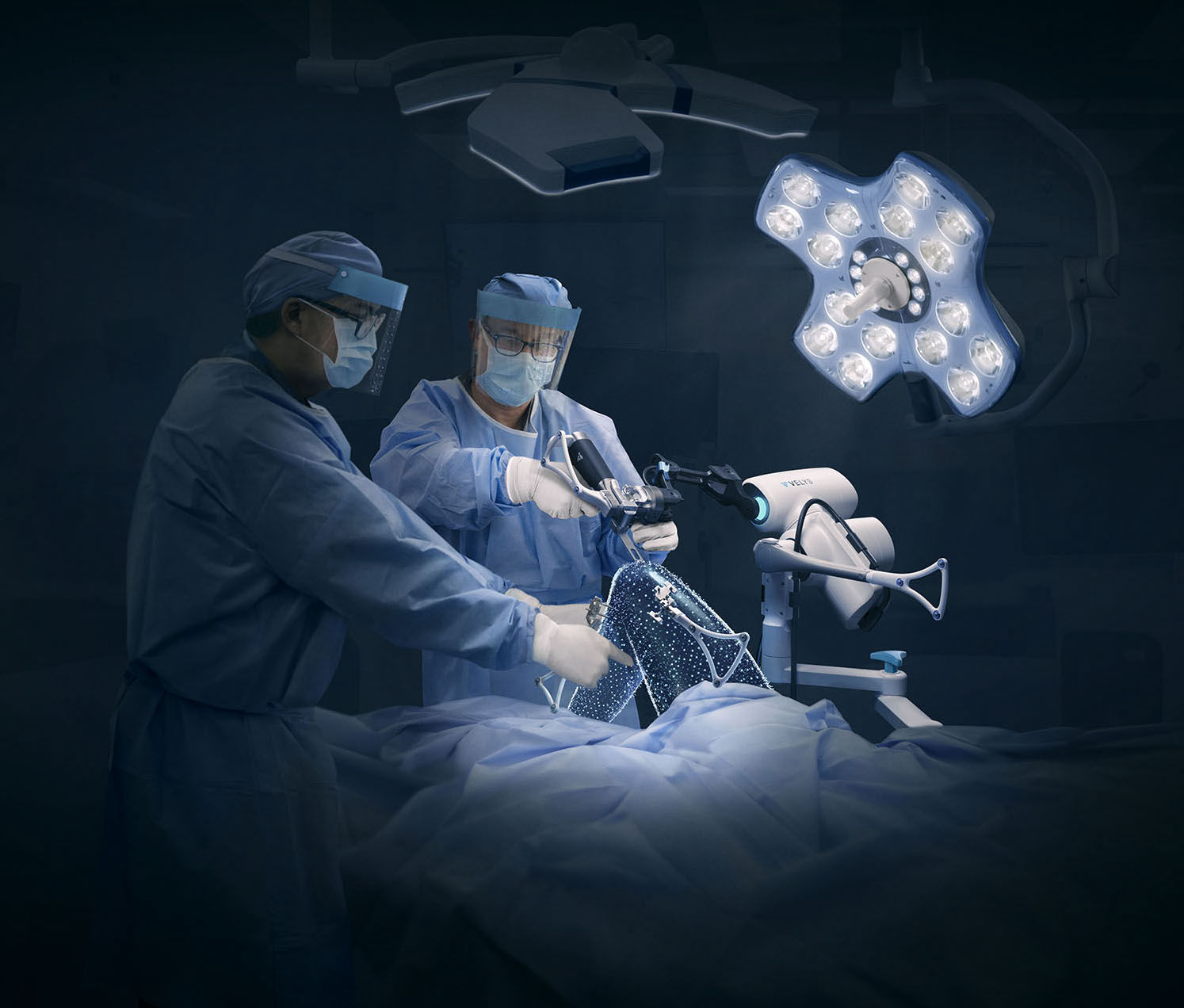
State-of-the-art support for knee osteoarthritis – precise, gentle, personalised
Are you suffering from painful knee osteoarthritis and considering a knee replacement?
We use innovative, robot-assisted surgical techniques with the VELYS™ system or patient-specific instruments with the MyKnee system. These methods allow for particularly precise implantation of the knee prosthesis – tailored to your individual anatomy. The high level of accuracy helps preserve surrounding tissue, improves mobility, and facilitates recovery.
Rely on our experience and advanced technology to regain a new quality of life with pain-free movement.